Update: On August 5, 2016, after an intense two-week trial, a jury in Alabama unanimously returned a verdict in favor of Caroline and JT Malatesta, with an award–including punitive damages–in the amount of $16 million (read about it here). The Malatestas’ attorney, Rip Andrews, said in his closing arguments, “We want corporations to know that reckless behavior will always be more expensive to them than safe behavior.” With this award, the jury sent that message.
You may have seen Caroline Malatesta’s story on Yahoo! Parenting. It’s a story that will hit home for a lot of people who have experienced maternity care mistreatment: Caroline says that the services and care she received at her hospital were vastly different from what was promised during her prenatal care. She ended up with a permanent nerve injury and chronic pain; she no longer has the ability to have sex or more children after she was, she alleges, wrestled on to her back during a “power struggle” with a nurse–as her baby’s head was forcefully held inside her for six minutes.
Caroline gave birth in Alabama, a place where women and advocates report hospital birth practices are decades behind research and the rest of the country; and where there are virtually no other options. There are no birth centers, and out-of-hospital midwifery care is illegal.
Here is Caroline’s story, in her words. When you’re done reading what she has to say, read what these nurses have to say about the abuse they’ve witnessed against women giving birth, and this piece about the dysfunction underlying so much of it.
I was 32 and pregnant with my fourth child when Brookwood Medical Center launched its marketing campaign for its new Women’s Center. I had delivered my first three babies at St. Vincent’s Hospital, its local competitor, and was planning to have my fourth baby there as well.
But I, like many other women in the community, found this new marketing campaign so captivating. It came from all angles – billboards, TV segments, news articles, websites, a blog, and even celebrity appearances. They were using phrases like “personalized birth plan,” “it’s about that birthing plan . . . whatever you want out of your birthing plan,” “a place that respects your birth plan,” “all about supporting and empowering women,” “all about comfort and choice,” “autonomy,” “We’re here to support each mom’s birth plan,” “wireless monitoring that will enable mothers to walk around during labor,” “[Wireless monitors] allow our patients to not be confined to their bed for the duration of their labor. They’re able to be mobile,” “a dedicated water birthing suite and amenities designed for natural child birthing plans,” and “staff trained extensively in assisting un-medicated delivery.”
No other hospital in town so much as mentioned such progressive concepts (and it should be noted that assisted out-of-hospital births aren’t legal here in Alabama).
This all came at a time when more of my friends around the country were beginning to have babies, and I was beginning to realize just how differently birth was handled elsewhere. Before then, I didn’t know there were options. I was hearing of friends being allowed to move around during labor, use the restroom, drink water, avoid stirrups, and birth in different positions. I always had been confined to the bed with a bedpan or catheter, only allowed to eat ice chips, and on my back in stirrups for delivery. I always was prepped from the waist down with surgical cloths and washed with antiseptic prior to delivery. I just figured that’s how childbirth was done everywhere. Lots of these friends had natural births, and talked about them positively. They didn’t have routine interventions and their recoveries seemed faster.
This sounded wonderful, and now these options were available to me! All I had to do was switch hospitals.
I interviewed an OB/GYN at Brookwood during my first trimester. He told me the interventions I received during my first three births were unnecessary and risky. He criticized routine use of the drug pitocin (medication to speed up labor and control hemorrhage). He said there was no need to be confined to the bed, not even during monitoring. He explained how laboring in upright positions alleviates pain, increases blood flow, helps position the baby properly, and opens up the pelvis. He told me research showed no benefit in continuous monitoring for low risk women like me; in fact, intermittent monitoring was recommended. He told me that letting the normal physiological process play out would be safest for my baby and me—which aligned with all of the research I’d been doing. Finally, after much thought and prayer, I switched hospitals during my 20th week of pregnancy. I hired a doula, read a big stack of birth books, exercised, and ate a healthy diet. I carefully made a birth plan based on best medical research, approved by my doctor. I was ready!
Fast-forward to the night of baby Jack’s birth in 2012. After laboring freely at home for several hours through some mild contractions, I arrived at the hospital and met my nurse. And that’s when it all started:
“Put on your gown and use the restroom now because you won’t be able to get out of bed for the next twenty minutes, and possibly for the rest of your labor.”
“But my doctor said I could labor however I wanted.”
“Well, your doctor’s not on call.”
What?! The contradiction between the marketing and the reality was so shocking that for a second I thought to myself, have I walked into the wrong hospital? I knew there was no medical evidence for what she was asking me to do. I asked her where the birth tub was because my birth plan included water birth, and she informed me my room didn’t accommodate a tub. I told her over and over that my doctor promised me I could walk around during monitoring, but she continued demanding I get in the bed on my back so she could hook me up to the wired monitor instead of the wireless one I was promised.
I begrudgingly got in the bed on my back, hoping my doula would arrive at any minute and rescue me from this nonsense. Baby Jack’s heartbeat ticked along perfectly on the monitor, but being on my back felt wrong and it hurt so much more than when I had been free to move. I continued asking why I had to be on my back and saying I needed to move around, but she ignored my questions and demanded I obey her, as if I were a disobedient child. I could sense my husband’s anxiety mounting. As we went back forth — me asking questions and telling her this was more painful for me, and her getting increasingly irritated — it became very clear that this wasn’t about health or safety. It was a power struggle.
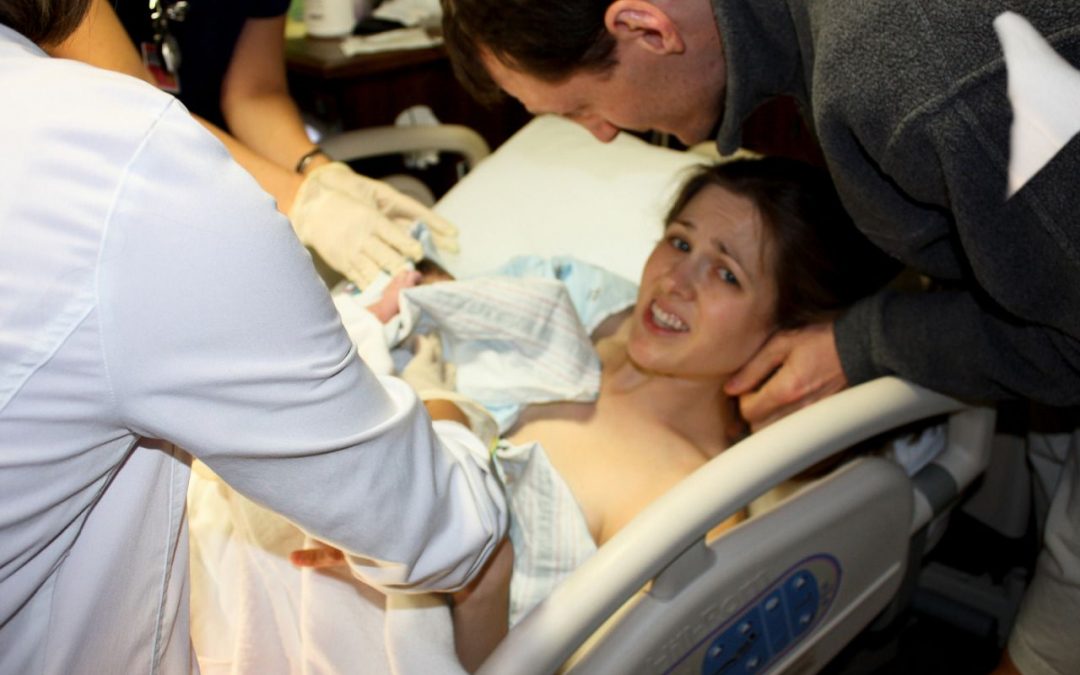
Suddenly, I felt a contraction coming on. I couldn’t bear the pain on my back any longer. I said “I can’t do this on my back!” and flipped over to my hands and knees. My water broke, and I realized the baby was crowning. My husband said, “I see his head!” I started arching my back while on all fours, and focused on slowly breathing out my baby. It all came so naturally—it felt right and safe and I knew my baby would be here any moment.
That’s when the nurse said, “Let’s get you on your back!” and everything went haywire. She grabbed my left wrist and forced it out from under me. I pulled back, but couldn’t escape her grip. She pulled my arm and rolled me over to my back. That is the moment I lost control over my birth. Forcing me to stay on my back was like forcing a person to hold their hand steady over an open flame – it was impossible for me to comply. The instinct to get off my back was overwhelming. I desperately tried to flip back to my hands and knees, struggling against the nurses to do so. The nurses held me down and pressed my baby’s head into my vagina to delay delivery as he was trying to come out.

“I was trying so hard to smile but I was in more pain than I’d been in during an unmedicated labor.”
It literally was torture. I screamed, “Stop!” to the nurses, but no one listened. The medical records summed up my reaction to the physical force quite well: “Unfortunately, the patient was not able to [act] in a controlled manner. She was pretty much all over the bed.” My doula ran in around this time. I looked at her in desperation and pled, “Help me!” but she could not. This went on for six minutes—me struggling, the nurses physically holding baby Jack in my body—when the doctor arrived. The nurse let go of baby Jack’s head, and he was born immediately into the doctor’s hands. I vividly remember the moment his head popped out. My right foot was planted firmly on the bed, elevating my hips as I tried to get off my back one last time, and a nurse was pushing my left leg awkwardly and asymmetrically toward my chest, causing me horrible pain.
So that’s how my precious child entered this world. As if birthing a baby isn’t hard enough, I gave birth while engaged in a physical struggle against the people I trusted to care for us.
To make matters worse, my first visitor was a lady from the billing department. There I was, having just given birth, and she walks in and says, “I’m here to talk to you about your bill.”
Despite the fact that Jack was a perfectly positioned little 6 lb 14 oz baby, and that I’ve delivered bigger babies at faster speed with no problem, I was injured badly. Because of the trauma I sustained from fighting while birthing, I now suffer from a permanent and debilitating nerve condition called Pudendal Neuralgia. My obstetrician called it the worst injury he has seen in all his decades of practice.
It has turned our family life upside down. I was a stay-at-home mother of four children, ages five and under, at the time Jack was born, and what happened to me during his birth left me unable to care for them as needed. I endure debilitating pain on a near daily basis—pain much worse than labor.

“My 6-year-old daughter took this picture of me on the floor. This is how I spent most of my days, fighting the pain from the nerve damage.”
I never had any psychological issues before the birth, but was diagnosed with PTSD afterwards. The panic attacks first set in when the nerve pain flared. I didn’t know what was happening to me. My skin would burn, I would hyperventilate, and I’d feel like I needed to escape my body. Something as simple as seeing a pregnant woman could set off an attack. I had dramatic dreams of being held hostage in a hospital while trying to escape a plot to murder me. Apparently, this was my brain’s way of trying to process what happened.
I especially struggled with feeling betrayed. I had trusted the hospital with one of the most important and sacred events in my life, and was left feeling chewed up and spit out. At first, I only confided these feelings in my husband. I was worried people would think I was being dramatic, because it’s not socially acceptable to complain about your birth if you have a healthy baby. It took a diagnosis of a permanent condition, and being so debilitated that I spent months on end in bed, for me to feel like I could openly acknowledge these feelings of betrayal and have them taken seriously. As I’ve opened up, other women in my community have come to me with their own stories of being misled or mistreated. I’m realizing this feeling of betrayal isn’t unique to me; it’s disturbingly common.
My husband struggles with the birth as well. He had prepared to be my cheerleader, not my bodyguard. He thought my nurse must have seen a serious problem when she used physical force on me, and that our child was in grave danger. He felt like a deer in headlights. There’s not a day that goes by that he doesn’t beat himself up for trusting the nurse.
In my quest for emotional healing, I sought answers from the hospital. But their patient ‘advocate’ cut off communication with me, saying, “Risk management and several key individuals have declined your request for a meeting. I am truly, truly sorry from the bottom of my heart about what you have been going through. I hope you have a good day. Someone has walked into my office for a meeting, and I have to go now.” Click. She hung up on me.
Out of basic self-respect, I couldn’t just leave it there. I grew up in a medical family, and filing a lawsuit wasn’t something I wanted to do, but the hospital left me no choice. After months of frustration and being stonewalled, my husband and I finally filed a lawsuit for medical negligence and fraud against Brookwood Medical Center and its parent company, Tenet Healthcare Corporation.
You hear the term “empowerment” thrown around a lot when people talk about birth. My hospital used that term in its own marketing. While my birth may have been the most disempowering experience in my life, standing up for myself and holding a large corporation accountable is the most empowering thing I’ve ever done.
Several aspects of litigation have been emotionally hard, including having to answer deeply personal and sexual questions in deposition and having my personal emails sifted through by attorneys. But the hardest part by far is sitting in depositions as a passive spectator, and listening to people try to justify their actions even in the face of my clear refusal. It’s a creepy feeling to hear nurses and hospital administrators who sincerely believe they have the rights over my body. But as a conscious and medically competent patient, the doctrine of informed consent guarantees that even in an emergency situation (which mine was not), a medical provider must respect my refusal of treatment, right? It doesn’t matter what my nurse thought would be best in that situation, or even why, because my ‘no’ is all that mattered – period. But I’m learning that’s not always how it works in the world of maternity care.
While the hospital doesn’t dispute the fact that there was no emergency or immediate danger in my situation, the phrase “safety of the mother and baby” has been repeated, almost reflexively, as if merely saying those words means no explanation is needed. I have yet to hear a single legitimate or medically sound answer as to why denying me mobility and forcing me to my back was safest. And that’s because there’s no medical evidence to support it.
My baby’s safety was always my top priority, which is precisely why I created a birth plan in the first place. Had my hospital simply respected that plan, as promised, I would be a healthy and functional mother today, and my family’s life would be very different. My husband and I love our baby more than anyone in the world loves him, and certainly more than anyone else in the delivery room that night. So it’s insulting to hear the hospital – the very people who were capable of treating me so badly, capable of violently forcing me to my back, and capable of shutting me out when I needed answers to process it all emotionally – now claim that concern for my baby’s and my wellbeing was the motive behind their actions. I could speculate about the hospital’s real motivations – efficiency, protocol, convenience, profit, liability, insurance, or a combination. I can’t say for sure what their top priority was, but it wasn’t the long-term wellbeing of my baby or me. My one and only priority was our health. And that’s why I was in the best position to make informed decisions about my care.

“It took everything in me to smile here. At Jack’s first birthday, we were living with my parents because I was unable to care for myself or my children. I went to the doctor in the morning, spent all day in bed, and got out of bed just for the birthday celebration.”
I’ve learned through this lawsuit that the doctors and nurses in my case hadn’t seen the marketing being shown to the rest of our community, and were not informed by the hospital about the promises being made about their services. The hospital didn’t have a way to know a woman was under the care of one of their doctors until she actually arrived at the hospital for delivery, much less have a way to communicate with doctors during pregnancy about accommodating her “personalized birth plan”—even though they specifically advertised that offering.
Contrary to the advertising, my nurses did not recall being “trained extensively in assisting un-medicated delivery.” Even worse, the expectations created by the hospital’s marketing directly contradicted their own policies. They claimed I wouldn’t be confined to the bed and could walk around, yet had a standing order for bed rest. They claimed I could choose how I wanted to be monitored, yet had a standing order for continuous monitoring. They claimed I could choose a water birth, yet the vast majority of their doctors didn’t offer it, and they had no control over who was on call. They even continued to advertise water birth for nearly three years after officially banning it in their facility! They claimed I could choose not to have medication, yet had a standing order for the drug Pitocin. Indeed, I learned after requesting my records that I was given Pitocin without my knowledge. The dosage given to me was listed right under the doctor’s documentation of my explicit refusal.
So many women, myself included, are told “it’s best to be flexible because birth is unpredictable.” I believe this is one of the most abused phrases in childbirth when it comes to railroading women’s choices. Yes, birth is unpredictable, and an outcome never can be guaranteed. But let’s not confuse a service with an outcome. No provider can guarantee a healthy birth outcome, but they can guarantee they will provide evidence-based services and supportive measures to give you the best chance at achieving a healthy birth. My son’s birth was straightforward—my maternity care was where the surprises came.
My hospital waited until the delivery room to start hashing out for the first time discrepancies between marketing promises and policies. Women were left to “negotiate” their birth plans while in active labor. At best, a woman would experience unnecessary anxiety – at worst, she would be forced physically to comply. It seems my hospital is blaming the unpredictability of their services on the unpredictability of birth.
As I was driving across town recently, I saw the words “I decide how to have my baby” plastered across a billboard in bold colors. It was an ad by my old hospital. They had ditched their baby-centered slogan “where babies come from” in favor of a trendier “woman-centered” slogan. My current hospital sold women “choice,” “empowerment,” and “autonomy,” and now my old hospital was selling women the ability to make their own healthcare decisions. It’s as if they think these are privileges granted to women instead of basic patient rights.
Seeing that sign, I felt sick to my stomach and helpless. It’s like I could see my nightmare of a story playing out all over again with some other unsuspecting woman.
When specifically asked, my doctor at my old hospital had been honest about the various interventions I would have to agree to. He gave me his practice group’s birth plan, a one-page document outlining these required interventions, including continuous monitoring, IV fluids, and a recumbent birth position. But had I seen that “group birth plan” after having seen the hospital’s current marketing as a new patient, I would have been blindsided, because I would have assumed that, indeed, I could decide how I have my baby – meaning interventions were a choice, not a requirement. Is it any wonder that women in my community come out of their births feeling lied to and betrayed?
Then we are made to feel selfish for being upset about our birth experience – as if we aren’t grateful for a healthy child – as if an experience and health are mutually exclusive instead of directly correlated. Just ask my family how important a mother’s health, both emotional and physical, is for the wellbeing of her children. It’s crucial. Any provider capable of treating a mother with disrespect cannot claim they are acting out of some magnanimous concern for her child. Caring about a child means caring for its mother.
As glitzy maternity marketing campaigns continue popping up around the country, I’m concerned more and more women will be enticed by mother-targeted campaigns that aren’t backed up by mother-centered care, as I unfortunately was. True mother-centered care starts with the boots-on-the-ground, not in the marketing department. It starts with hospitals instilling a culture of respect for the birthing woman and the birthing process. It starts with transparency, evidence-based care, and collaborative care. And it results in better outcomes. Unfortunately, this doesn’t seem to be the norm where I live, and until it is, “autonomy,” “choice” and “empowerment” are nothing but empty promises.
I may have little chance of making a real difference in the way large corporations and hospitals market maternity care. Who knows. But I’m hoping that maybe – just maybe – my lawsuit will make them think twice about lying to women giving birth.
// Caroline Malatesta
Read more about what some nurses have to say about the abuse they’ve witnessed against women giving birth, and the dysfunction underlying so much of this mistreatment.
 A former communications strategist at a top public affairs firm in Baltimore, Maryland, Cristen Pascucci is the founder of Birth Monopoly, co-creator of the Exposing the Silence Project, and, since 2012, vice president of the national consumer advocacy organization Improving Birth. In that time, she has run an emergency hotline for women facing threats to their legal rights in childbirth, created a viral consumer campaign to “Break the Silence” on trauma and abuse in childbirth, and helped put the maternity care crisis in national media. Today, she is a leading voice for women giving birth, speaking around the country and consulting privately for consumers and professionals on issues related to birth rights and options.
A former communications strategist at a top public affairs firm in Baltimore, Maryland, Cristen Pascucci is the founder of Birth Monopoly, co-creator of the Exposing the Silence Project, and, since 2012, vice president of the national consumer advocacy organization Improving Birth. In that time, she has run an emergency hotline for women facing threats to their legal rights in childbirth, created a viral consumer campaign to “Break the Silence” on trauma and abuse in childbirth, and helped put the maternity care crisis in national media. Today, she is a leading voice for women giving birth, speaking around the country and consulting privately for consumers and professionals on issues related to birth rights and options.
Consult with Cristen | Resources + more Articles
Free handouts + monthly-ish updates from Birth Monopoly: click here